Principles
This procedure combines a significant reduction of the stomach with low risk of malabsorption by creating a gastric pouch, where food arrives, separated from the rest of the stomach.
The proximal part of the small bowel is then divided in two. The lower segment (Roux’s food loop) is attached to the small gastric pouch and the upper segment (bilio-pancreatic loop) attached further down the Roux loop.
The food thus passes from the gastric pouch into the initial part of the intestine by bypassing not only most of the stomach but also the duodenum and the first jejunal loops (50 to 70 cm) which disrupts digestion and absorption of food.
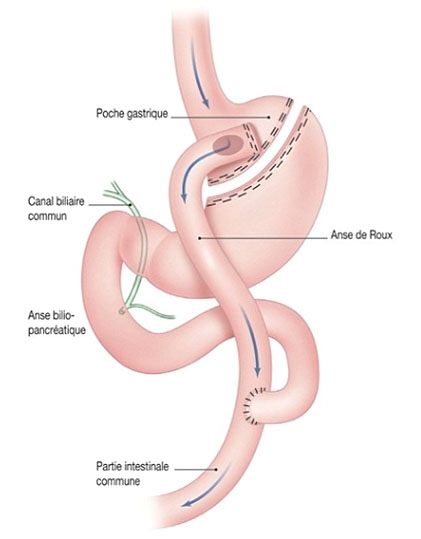
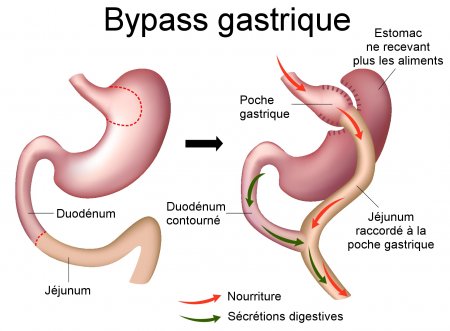
After a Roux-en-Y gastric bypass, several mechanisms contribute to induce weight loss:
– A decrease in the feeling of hunger linked to the decrease of Ghrelin (hormone stimulating appetite) but less than after a sleeve gastrectomy,
– A decrease in gastric capacity,
– A very accelerated gastric emptying associated with the short-circuit of the pylorus causing earlier secretion of satiety hormones (PYY and GLP1),
– A malabsorption that mainly affects fats and to a lesser degree proteins,
– Finally an aversive reaction to sugary foods in the case of dumping syndrome.

Benefits
- No foreign body implantation
- Good weight loss
- Remission of Type 2 Diabetes Regardless of Weight Loss
- Reversible in case of complication (but weight gain after reversion)
Disadvantages
-
The excluded stomach, duodenum and bile ducts are inaccessible to endoscopy.
-
Malabsorption requires lifetime supplementation of vitamins and trace elements and can affect the effectiveness of drug treatments.
-
The excluding pylorus puts you at high risk of late dumping syndrome and hypoglycemia.
-
The creation of the Y loop exposes you to the risk of occlusions on internal hernias.
-
In cases of long-term weight regain, there are few satisfactory solutions.

